Exercises For Back Pain
Pain-Relief Exercise: The Lower Back
By Marc Heller, DC
Specific exercises are a powerful tool for acute pain relief. These exercises are specific for sciatica or discogenic low back pain, and can help almost any acute lower back pain. Exercise has many purposes, including increasing strength and flexibility and improving posture, but the focus here is on exercises that are safe and useful for acute pain relief.
Many of your patients may be afraid to exercise when they are in pain, or they may have hurt themselves while exercising. Pain-relief exercise has to be very specific and be done properly; it also has to be the proper exercise. McKenzie1,2 has led the way here, giving us a basic principle of mechanical testing and a set of simple exercises for back pain.
The basic principle for pain-relief exercise is that the patient should feel better after he or she has finished the exercise. It may be somewhat difficult or slightly painful to do the exercise, but that is OK if the patient feels better afterward. It is ideal for you, as the doctor, to show the patient these exercises in the office, as proper technique is critical, and you can help get the patient through any fear of movement. Having something that the patient can do when in pain, and that relieves his or her pain, is very empowering to the patient. It also helps address the depression and helplessness that accompanies severe pain.
Let’s start with McKenzie extension. If the patient has low-back or leg pain, made worse by flexion, made worse by repetitive flexion, or caused by a flexion motion, he or she will probably benefit from extension. Lumbar extension can be done prone, and looks a lot like the yoga Cobra or Sphinx pose. Leave the lower half of the body on the floor, and use your arms to lift the upper body. McKenzie teaches this as a passive motion, using the upper body to lift the trunk.
Others from the yoga and Pilates world add core contraction, firing the transverse abs, the pelvic floor, and the multifidi while lifting the upper body. This more active form probably is only useful if the patient already understands abdominal co-contraction, as it’s a bit complex to teach to someone in severe pain. A variation on this can be done standing, with the patient putting his or her fists on their lower back and bending backward.
Bookhout3 has added another variation to this; if one side of the lower lumbars or the sacral base is more stiff than the other on palpation, modify the lumbar extension, leaving the stiff side on the table and flexing forward the opposite leg. See the picture below. I call it “one-legged press-ups.” The only tricky thing about this one is that it cannot be done on the floor; the patient needs to use a table or bench. A bed is a bit too soft, but it can work if that is the only available tool. Again, the simple test: Does it feel OK during the motion; does it feel better afterward?
These exercises are designed to be held for a few seconds; then returned to the beginning position and repeated. McKenzie recommends 10 repetitions. The patient in acute pain should repeat these exercises hourly at first. As he or she recovers, decrease frequency.
The next exercise I teach is the pelvic tilt, again modified for pain. The picture below (see page 42) shows it supine, but it also can be done sitting or on all fours. Most of you are familiar with this. Some of your patients will understand this isolated pelvic motion easily; others will have a hard time with it. The key instruction in the flexion direction is to “curl your tailbone up, flattening your spine toward the floor.” The key instruction for the anterior pelvic tilt, extension direction is to “push your tailbone down to the floor, as you arch your back gently upward off the floor.”
The modification for acute pain is to go only as far as you can in either direction without causing pain. The patient needs to learn to “feather” the motion in the difficult direction, going only to the edge of the pain, not causing a sharp spasm each time. The patient will be pleasantly surprised to feel the mobility gradually increase as the exercise is repeated. This can be thought of as a micro-movement, useful for getting motion back into an extremely stiff area, and bringing nutrients and afferentation back to an area that has been inflamed and stiff. This exercise should be done alternately in both directions, with at least 10 full repetitions, possibly more. It should be used frequently when the patient is in pain or feeling stiff. It is also a good exercise to do gently before getting out of bed in the morning.
I’ll describe one more position. This is not really an exercise, but a position of rest. It is well-pictured in an article on Dr. Craig Liebenson’s Web site.2 It involves lying on the back on a carpeted or padded floor, with the legs in a 90/90 position, resting on a chair. I call this “going to Tahiti,” with the idea being taking a mini-vacation in your mind. The patient can use this just to rest his or her back, and/or use it as a position for icing the back.
The last exercise is a bit more complex, but worth it. I use it as a reset exercise, whenever my patient’s (or my own) back feels “off.” I call it the “spine-lengthening squat.” It is a yoga exercise, with various names in yoga. What I love about it is that the spine is in neutral, you are firing the core, and you are lengthening and decompressing the spine. I think there is something very special about any exercise that combines these three factors.
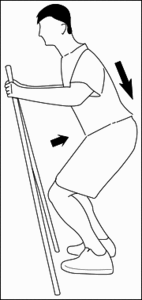
Here are the steps for this one. Begin by squatting down, as far as you are comfortable, pushing your bottom way backward. Your hands can be in any one of the three positions pictured below. The easiest is with your hands on your thighs; the most difficult is with your hands raised. Your knees are hip-width apart, and you isometrically pull them together.
Ideally, use a yoga block, or some other 6-8 inch-wide firm rubber or plastic object, and push your knees together into this. Pull the belly in while keeping your back in a neutral, lordotic position. Now, imagine you are sinking your tailbone toward the ground, lengthening your spine. Don’t move more than half an inch; it is an almost isometric action. Once you are set in the position, check yourself, knees isometric inward, core-belly isometrically pulled in, maintaining lumbar lordosis, tailbone isometric lengthening toward the floor. If you are using the sticks, or raising your arms, you also can imagine a lift of the whole upper body upward. Hold for 10-60 seconds, and then come slowly out. Repeat 2-3 times. A yoga instructor could show you the subtleties of this better than I can describe here.
Now, a bit of a personal story here: A couple of months ago, I reinjured my L5 disc while sneezing. I was stuck in flexion and had bad pain for several days. I would use the spine-lengthening squat every time I got up from sitting, as sitting put me back into a flexion antalgia, and this exercise took me immediately to an upright posture. This really helped me, I don’t know how patients who do not have these skills cope, but I know they would need way more pain meds.
Teaching your patient how to deal with pain episodes is an incredibly valuable skill; I hope you take the time to do this. Ideally, the doctor should use all of the tools at your command in these cases, including postural advice, low-force adjustments and traction, ice, exercise, nutraceutical anti-inflammatories, and coordinate care for pharmaceuticals if needed.
References
- McKenzie RA, The Lumbar Spine: Mechanical Diagnosis and Therapy. New Zealand; Spinal Publications, Inc., 1981.
- Web site of Dr. Craig Liebenson: www.lasportsandspine.com.
- Bookhout, Mark. “Exercise as an Adjunct to Manual Medicine” (seminar), 1998.